Few Thought He'd Survive the Night, But after 77 days, Temple's Most Critical Amtrak Patient Finally Went Home

Three weeks after the crash of Amtrak train 188, Aaron Levine, 80, woke up in Temple University Hospital’s intensive care unit.
He was on a ventilator. He had nine broken ribs, which had punctured his right lung, collapsing it. The area around his lung had filled with blood. He had spinal fractures and a broken collarbone.
He took so long to wake up, doctors had worried about brain injury.
Unable to speak because of the breathing tube, he mouthed the words to family, nurses, doctors, everyone:
“Let me die.”
Levine, one of 238 passengers on that train, happened to be a personal injury lawyer who lived in Washington, D.C. He had spent the last 50 years suing hospitals, doctors and drug companies. He had no confidence in medicine’s ability to bring him back.
Amy J. Goldberg, a trauma surgeon at Temple for 23 years, chair of the department of surgery, who had spent the last three weeks with so many others fighting to save him, stood at his bedside.
“I hope you have a good lawyer,” he told her, mouthing the words. “You’re going to need one.”
The train derailed just before 9:30 p.m. on May 12, exactly one year ago today. Fifty-four passengers, more than at any other Philadelphia hospital, were treated at Temple, 24 of them admitted. Levine was the most critical. One passenger, in his 40s, with similarly severe chest injuries and also pelvic injuries, had died within a few hours of the crash.
Levine and his wife, Barbara, 78, art lovers and collectors, were on their way to New York that night for the Frieze art fair, and then to Europe for a month.
They were riding in the quiet car, the second car, in the last seat, facing Washington. They rode the train often and liked that seat, because it had legroom. Aaron was against the window, his wife next to him.
“I got totally thrown to the other side of the train,” said Barbara. “I was screaming for him but there was no answer. I couldn’t see. I was helped out of the train by rescue workers.”
“I had five cracks in my pelvis,” she added. “They took me in a police van to Hahnemann. You know the potholes in the road? I could have had ten more cracks in my pelvis.” She still had her handbag, and her phone, and from the back of the van called her son, Andrew Levine, 54, a physician in Manhattan, who spent 12 years as an ER doctor.
He got a car, got to Temple by midnight, and went and found his father in the trauma bay.
“There was a whole trauma team around him with 10 bags of different blood products, IV medications,” recalled Andrew. “He looked like death. He was sedated. On a respirator. His face was bruised and swollen and he didn’t look anything like himself.”
The son paused repeatedly, overcome with emotion.
“He was on blood thinners already because he’d had a small stroke five years ago. So he probably almost bled to death. When I saw him in the trauma bay, my first instinct was it’s all over.”
When they wheeled his father from emergency to the ICU, after 2 a.m., he went and checked on his mother at Hahnemann. He couldn’t bring himself to tell her he thought his father was going to die, and left a little room for hope. He had just checked into a hotel, at 5 a.m., when Dr. Goldberg called him, “and told me they were starting a medication, Levophed. It’s used when you can’t maintain your blood pressure anymore. It’s like a last ditch effort. Without putting words in her mouth, I felt like that was her giving me another sign that he wasn’t going to make it.”
• • •
To the surprise of many doctors and nurses, Aaron Levine survived that first night.
Barbara Levine was transferred the next day from Hahnemann to Temple, to a room down the hall from her husband and the ICU.
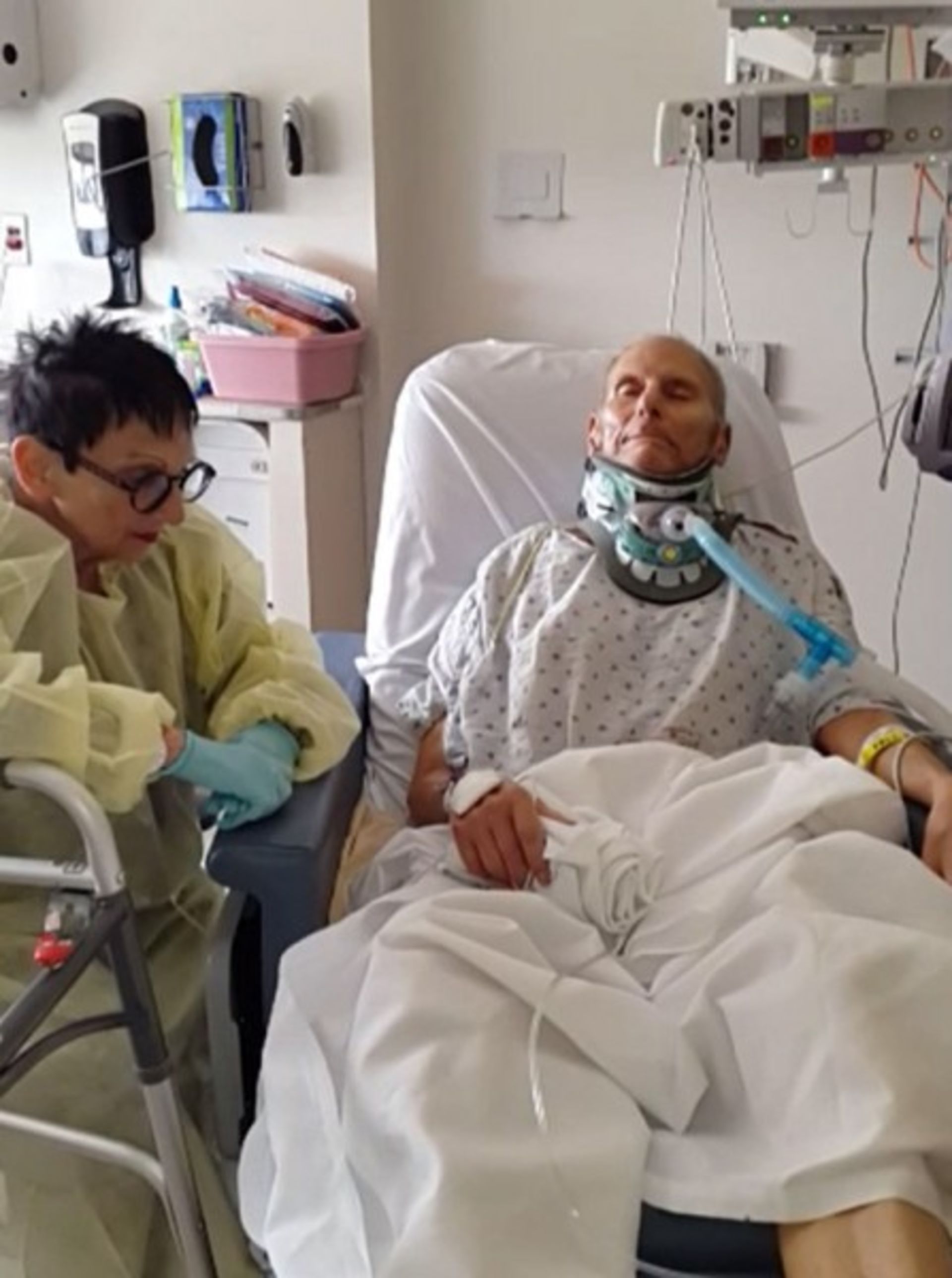
After five days, Barbara Levine was discharged, got a wheel-chair accessible hotel room in Center City, and came to Temple every day. One of her three children was there virtually every day as well.
Aaron Levine presented an immense medical challenge. So many things were working against him – his age, the severity of his injuries, the fact that he was on blood thinners. Levine was sedated, put into an induced coma. The pain from his broken ribs would have been unbearable, and he needed to be absolutely still. If he moved at all, his oxygen level would plunge.
His situation was truly precarious. And on the fourth day, he got pneumonia.
After two weeks, doctors tried bringing him out of the coma, but he didn’t wake up. They feared brain injury.
As his daughter, Jennifer Levine, who had flown in from Chicago, said, “Every new phase brought a new fear.”
And when he finally awoke, and realized the extent of his injuries, he so badly wanted to die.
Lying in on the 9th floor of Temple hospital, he thought he’d never again have a life worth living.
Levine told his son Andrew, the physician, to look up the Oregon assisted suicide law, “because I planned to go there.”
Andrew refused.
“Well then I’m going out the window.”
“You can’t get to the window,” his son replied.
The Levine children were equally adamant. This wasn’t cancer. This wasn’t stroke. This was trauma, and he could recover.
Levine’s desire to die made it difficult on doctors, who had worked so hard to save him. He’d already come so far.
“He told his family to let him die and we were really challenged by that,” said Goldberg.
Every step forward was followed by a step back, it seemed. He got pneumonia three times, plus many other infections, said his son. “It was a real challenge to regulate his pain,” said his daughter. “He was so uncomfortable. They were always giving him different medications that would have different effects. He would be nauseous, or his stomach hurt, or he’d sleep all day.”
He weighed 191 pounds on admission. Even with a feeding tube, his weight began to plunge. Six weeks later, on June 23, he was 143.
Getting him to breathe again on his own, off the ventilator, was an immense challenge. He couldn’t get enough oxygen without it.
Even though he was miserable, Aaron Levine always looked forward to physical therapy with Carrie Dempsey and her colleagues.
On June 1, they got him to sit up on the bed for the first time, for about 10 minutes. On June 5, he stood for a moment, with a physical therapist on each arm. By June 18, he could get out of bed and sit in a chair.
“They were like a cheering squad,” he said of his therapists.
As he gained strength, Levine started making jokes. Staff may not have loved his jokes, but loved that he was making them, becoming himself again. Dempsey, one of his physical therapists, was pregnant, and when she’d leave early for a doctor’s appointment, he’d ask the next day, “how’s the baby?”
In early July, Rebecca Armbruster, then the associate chief medical officer, who visited every Amtrak patient every day, and who had become quite close to the Levine family, brought her two young daughters to visit Levine. Doctors had performed a tracheostomy, and the breathing tube was now connected through his throat. This enabled him to talk softly. Armbruster asked Levine to give her daughters some advice. He gestured for the two girls to come closer, smiled, and whispered, “Stay away from trains.”
Also in that first week of July, nurses and residents clapped when he walked out of his room for the first time, a wheelchair in front and another in back, a therapist on each arm. He needed a portable ventilator to walk, still too weak to breathe on his own. “The noise of the machine made him anxious,” said Dempsey. “He feared it would break.”
Finally, by July 8 – 57 days since the crash – he was off the breathing machine for good, able to eat a pureed diet. He was 132 pounds.
• • •
The Levine children were frustrated with Amtrak. They felt it provided little help getting their mother a hotel room, a wheelchair for her and a van that could transport her in a wheelchair to Temple every day. They wanted a physical therapist to go to her hotel, just as if she were getting care at home.
“Everything that happened to support of my parents happened because my brothers and I or Temple arranged it,” said Jennifer Levine.
Having a patient in the ICU for so long – especially considering the circumstances – was stressful on family and staff. When Aaron Levine was suicidal, the family wanted an aide in the room fulltime, in case he tried to harm himself, and it was a struggle at first to get one, Jennifer Levine said. When the children wanted a cot for Barbara Levine, so she could rest during the day when she visited her husband, Shirley Defrehn, the case manager, who worked hard to make life as easy as possible on the family, had to explain there simply was no place to put it.

“Shirley Defrehn and Rebecca Armbruster were amazing in terms of being very open to collaboration and receptivity, and being responsive,” said Jennifer Levine. “So in terms of our experience, that made such a huge difference. Dr. Armbruster, you would email her and she would respond in a thoughtful, problem-solving way almost immediately. As opposed to having to hunt someone down and convince them why to care.”
The weeks dragged on. Every other Amtrak patient had been discharged.
By the mid-July, even Barbara Levine had reached her limit.
“On the corner by the hotel is a Rite Aid,” she recalled. “A bag lady was sitting outside the drug store all the time. She’d been watching me go from a wheelchair to a walker to a cane. One day she said to me, ‘I can’t believe what progress you’ve made.’ I knew it was time for us to go home.”
• • •
And finally that day came, July 28. With help, and portable oxygen, he could walk the length of the ICU. His weight was up to 137. Defrehn had made arrangements for him to go by ambulance to a rehabilitation hospital in Washington. His wife and three children and grandchildren were all there to see him leave. He was still frail – in his own words, “decrepit.” There was great concern whether he could he make it all the way to Washington. His son the physician would ride with him.
It was an anxious moment, but still a triumphant one. “A miracle,” said his wife. Defrehn, the case manager, cried.
In August, Goldberg, who as Temple’s top trauma doctor had guided Levine’s care, went to Washington to check out a blood refrigerator she was thinking of buying for the operating room. She visited the patient who had once threatened to sue her. It was his last day of rehabilitation.
“Dr. Goldberg was wonderful,” he says now. “She saved my life. She called the shots.”
In December, Aaron Levine sent a case of champagne for the holidays to Shirley Defrehn at Temple and told her to give bottles to the physicians, nurses and therapists who had helped him heal. Defrehn kept one bottle for herself but won’t drink it. Goldberg won’t drink hers, either. They want to keep that bottle to remember. Temple helped this man who wanted to die get better, and go home.
• • •
Epilogue:
A year after the crash, Levine is home and working again, though he says, “I can’t try a case anymore. I can’t go to court anymore.” He is winded walking up steps, and can’t walk very far without having to rest. He also can’t raise his arms high enough to put on his own jacket. And because of medications he was on in the ICU, his blood pressure is lower now. So no more cigars or alcohol.
“I used to love my martinis,” he laments.
“Strangely enough,” he adds, “There’s a kind of a benefit to all of this. It refocuses you on what’s important in life.”
Within limits, the Levines are back to traveling a bit, going to art shows and galleries in New York. With one exception.
“We don’t take the train anymore,” he says. “We hire a driver.”
• • •
Michael Vitez, winner of the 1997 Pulitzer Prize for Explanatory Journalism at The Philadelphia Inquirer, is the director of narrative medicine at the Lewis Katz School of Medicine at Temple University. Michael.vitez@temple.edu
